WO2014158242A1 - Method for the treatment of fatty liver disease - Google Patents
Method for the treatment of fatty liver disease Download PDFInfo
- Publication number
- WO2014158242A1 WO2014158242A1 PCT/US2013/072092 US2013072092W WO2014158242A1 WO 2014158242 A1 WO2014158242 A1 WO 2014158242A1 US 2013072092 W US2013072092 W US 2013072092W WO 2014158242 A1 WO2014158242 A1 WO 2014158242A1
- Authority
- WO
- WIPO (PCT)
- Prior art keywords
- group
- fatty liver
- compound
- liver disease
- alkyl
- Prior art date
- Legal status (The legal status is an assumption and is not a legal conclusion. Google has not performed a legal analysis and makes no representation as to the accuracy of the status listed.)
- Ceased
Links
- LJTSIMVOOOLKOL-NXGXIAAHSA-N CC(C(C/C=C(\C)/CC/C=C(\C)/CCC=C(C)C)C(C(OC)=C1OC)O)C1=O Chemical compound CC(C(C/C=C(\C)/CC/C=C(\C)/CCC=C(C)C)C(C(OC)=C1OC)O)C1=O LJTSIMVOOOLKOL-NXGXIAAHSA-N 0.000 description 1
- 0 CC(C*)=CCC(C(*)C(C(**)=C1**)=O)C1O* Chemical compound CC(C*)=CCC(C(*)C(C(**)=C1**)=O)C1O* 0.000 description 1
Classifications
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61K—PREPARATIONS FOR MEDICAL, DENTAL OR TOILETRY PURPOSES
- A61K31/00—Medicinal preparations containing organic active ingredients
- A61K31/12—Ketones
- A61K31/122—Ketones having the oxygen directly attached to a ring, e.g. quinones, vitamin K1, anthralin
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61K—PREPARATIONS FOR MEDICAL, DENTAL OR TOILETRY PURPOSES
- A61K31/00—Medicinal preparations containing organic active ingredients
- A61K31/56—Compounds containing cyclopenta[a]hydrophenanthrene ring systems; Derivatives thereof, e.g. steroids
- A61K31/575—Compounds containing cyclopenta[a]hydrophenanthrene ring systems; Derivatives thereof, e.g. steroids substituted in position 17 beta by a chain of three or more carbon atoms, e.g. cholane, cholestane, ergosterol, sitosterol
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61K—PREPARATIONS FOR MEDICAL, DENTAL OR TOILETRY PURPOSES
- A61K36/00—Medicinal preparations of undetermined constitution containing material from algae, lichens, fungi or plants, or derivatives thereof, e.g. traditional herbal medicines
- A61K36/06—Fungi, e.g. yeasts
- A61K36/07—Basidiomycota, e.g. Cryptococcus
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61K—PREPARATIONS FOR MEDICAL, DENTAL OR TOILETRY PURPOSES
- A61K9/00—Medicinal preparations characterised by special physical form
- A61K9/0012—Galenical forms characterised by the site of application
- A61K9/0053—Mouth and digestive tract, i.e. intraoral and peroral administration
- A61K9/0056—Mouth soluble or dispersible forms; Suckable, eatable, chewable coherent forms; Forms rapidly disintegrating in the mouth; Lozenges; Lollipops; Bite capsules; Baked products; Baits or other oral forms for animals
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61K—PREPARATIONS FOR MEDICAL, DENTAL OR TOILETRY PURPOSES
- A61K9/00—Medicinal preparations characterised by special physical form
- A61K9/0012—Galenical forms characterised by the site of application
- A61K9/007—Pulmonary tract; Aromatherapy
- A61K9/0073—Sprays or powders for inhalation; Aerolised or nebulised preparations generated by other means than thermal energy
- A61K9/0078—Sprays or powders for inhalation; Aerolised or nebulised preparations generated by other means than thermal energy for inhalation via a nebulizer such as a jet nebulizer, ultrasonic nebulizer, e.g. in the form of aqueous drug solutions or dispersions
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61K—PREPARATIONS FOR MEDICAL, DENTAL OR TOILETRY PURPOSES
- A61K9/00—Medicinal preparations characterised by special physical form
- A61K9/48—Preparations in capsules, e.g. of gelatin, of chocolate
- A61K9/4841—Filling excipients; Inactive ingredients
- A61K9/4875—Compounds of unknown constitution, e.g. material from plants or animals
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61P—SPECIFIC THERAPEUTIC ACTIVITY OF CHEMICAL COMPOUNDS OR MEDICINAL PREPARATIONS
- A61P1/00—Drugs for disorders of the alimentary tract or the digestive system
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61P—SPECIFIC THERAPEUTIC ACTIVITY OF CHEMICAL COMPOUNDS OR MEDICINAL PREPARATIONS
- A61P1/00—Drugs for disorders of the alimentary tract or the digestive system
- A61P1/16—Drugs for disorders of the alimentary tract or the digestive system for liver or gallbladder disorders, e.g. hepatoprotective agents, cholagogues, litholytics
-
- A—HUMAN NECESSITIES
- A61—MEDICAL OR VETERINARY SCIENCE; HYGIENE
- A61P—SPECIFIC THERAPEUTIC ACTIVITY OF CHEMICAL COMPOUNDS OR MEDICINAL PREPARATIONS
- A61P43/00—Drugs for specific purposes, not provided for in groups A61P1/00-A61P41/00
Definitions
- the present invention relates to a method for the treatment of fatty liver disease, and more particularly, to a method of administering a cyclohexenone compound.
- Fatty liver refers to a pathogenic condition where fat comprises more than 5% of the total weight of the liver. Fatty liver and steatohepatitis are frequently found in people who intake excessive alcohols and who have obesity, diabetes, hyperlipidemia, etc.
- NAFLD nonalcoholic fatty liver disease
- steatosis simple fatty liver
- NASH nonalcoholic steatohepatitis
- cirrhosis irreversible, advanced scarring of the liver. All of the stages of NAFLD have in common the accumulation of fat (fatty infiltration) in the liver cells (hepatocytes).
- NASH the fat accumulation is associated with varying degrees of inflammation (hepatitis) and scarring (fibrosis) of the liver.
- the NAFLD spectrum is thought to begin with and progress from its simplest stage, called simple fatty liver (steatosis). That is, fatty liver is the initial abnormality in the spectrum of NAFLD. Simple fatty liver involves just the accumulation of fat in the liver cells with no inflammation or scarring. The fat is actually composed of a particular type of fat (triglyceride) that accumulates within the liver cells. Fatty liver is a harmless (benign) condition.
- the next stage and degree of severity in the NAFLD spectrum is NASH. As mentioned, NASH involves the accumulation of fat in the liver cells as well as inflammation of the liver.
- the inflammatory cells can destroy the liver cells (hepatocellular necrosis).
- steatohepatitis and “steatonecrosis”
- steato refers to fatty infiltration
- hepatitis refers to inflammation in the liver
- necrosis refers to destroyed liver cells.
- NASH in contrast to simple fatty liver, is not a harmless condition. This means that NASH can ultimately lead to scarring of the liver (fibrosis) and then irreversible, advanced scarring (cirrhosis). Cirrhosis that is caused by NASH is the last and most severe stage in the NAFLD spectrum.
- the invention provides a method of treating, inhibiting and/or preventing fatty liver disease in a patient in need thereof, comprising administering an effective amount of a cyclohexenone compound of the formula (I) as described herein to said patient.
- the cyclohexenone compound is administered with a second ingredient.
- [0006] provides methods of treating, inhibiting and/or preventing fatty liver disease in a patient in need thereof, comprising administering an effective amount of a cyclohexenone com ound of the following formula (I) to said patient,
- each of X and Y independently is oxygen, NR 5 or sulfur;
- each of Ri, R 2 and R 3 independently is a hydrogen, methyl or (CH 2 ) m — CH 3 ;
- each of R 5 and Re is independently a hydrogen or C j -C 8 alkyl
- R 7 is a C r C 8 alkyl, OR 5 or NR 5 R 6 ;
- n l-12; or a pharmaceutically acceptable salt, metabolite, solvate or prodrug thereof.
- FIG. l(A-D) shows representative photomicrographs of HE-stained sections of livers of Group A (vehicle control) and Group B (test compound, Compound 1) in a Fatty Liver Disease model.
- FIG. 1(A) and 1(B) show HE-stained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 200 X, respectively.
- FIG. 1(C) and 1(D) show HE-stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 200 X.
- FIG. 2(A-D) shows representative photomicrographs of Sirius-red stained sections of livers of Group A and Group B Fatty Liver Disease model.
- FIG. 2(A) and 2(B) show Sirius-red stained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 200 X, respectively.
- FIG. 2(C) and 2(D) show Sirius-red stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 200 X.
- FIG. 3(A-D) shows representative photomicrographs of collagen Type 3- immunostained sections of livers of Group A and Group B Fatty Liver Disease model.
- FIG. 3(A) and 3(B) show collagen Type 3-immunostained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 400 X, respectively.
- FIG. 3(C) and 3(D) show Sirius-red stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 400 X.
- FIG. 4 shows diagrams of the whole blood glucose concentration (mg/dL) of Group A and Group B.
- FIG. 5 shows diagrams of the plasma triglyceride concentration (mg/dL) of Group A and Group B.
- FIG. 6 and FIG. 7 respectively show diagrams of plasma AST and plasma ALT concentration (U/dL) of Group A and Group B.
- FIG. 8(A-D) shows representative photomicrographs of HE-stained sections of livers of Group A and Group B regarding fibrosis of steatohepatitis liver cells.
- FIG. 8(A) and 8(B) show HE-stained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 200 X, respectively.
- FIG. 8(C) and 8(D) show HE-stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 200 X.
- FIG. 9(A-D) shows representative photomicrographs of Sirius-red stained sections of livers of Group A and Group B regarding fibrosis of steatohepatitis liver cells.
- FIG. 9(A) and 9(B) show Sirius-red stained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 200 X, respectively.
- FIG. 9(C) and 9(D) show Sirius-red stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 200 X.
- FIG. lO(A-D) shows representative photomicrographs of collagen Type 3- immunostained sections of livers of Group A and Group B regarding fibrosis of steatohepatitis liver cells.
- FIG. 10(A) and 10(B) show collagen Type 3-immunostained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 400 X, respectively.
- FIG. 10(C) and 10(D) show Sirius-red stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 400 X.
- FIG. 11 shows diagrams of the whole blood glucose concentration (mg/dL) of Group A and Group B.
- FIG. 12 shows diagrams of the plasma triglyceride concentration (mg/dL) of Group A and Group B.
- FIG. 13 and FIG. 14 respectively show diagrams of plasma AST and plasma ALT concentration (U/dL) of Group A and Group B.
- FIG. 15(A-F) shows representative photomicrographs of HE-stained sections of livers in a fatty liver condition assay in Group A (vehicle control), Group B (test compound & ergosterol) and Group C (test compound alone).
- FIG. 15(A) and 15(B) show HE-stained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 200 X, respectively.
- FIG. 15(C) and 15(D) show HE-stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 200 X.
- FIG. 15(E) and 15(F) show HE-stained sections of livers of Group C at an enlargement ratio of 50 X enlargement ratio of 200 X.
- FIG. 16(A-F) shows representative photomicrographs of Sirius-red stained of livers from Group A to Group C.
- FIG. 16(A) and 16(B) show Sirius-red stained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 200 X, respectively.
- FIG. 16(C) and 16(D) show Sirius-red stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 200 X.
- FIG. 16(E) and 16(F) show Sirius-red stained sections of livers of Group C at an enlargement ratio of 50 X enlargement ratio of 200 X.
- FIG. 17(A-F) shows representative photomicrographs of collagen Type 3- immunostained sections of livers from Group A to Group C.
- FIG. 17(A) and 17(B) show collagen Type 3-immunostained sections of livers of Group A at an enlargement ratio of 50 X enlargement ratio of 400 X, respectively.
- FIG. 17(C) and 17(D) show Sirius-red stained sections of livers of Group B at an enlargement ratio of 50 X enlargement ratio of 400 X.
- FIG. 17(E) and 17(E) show Sirius-red stained sections of livers of Group C at an enlargement ratio of 50 X enlargement ratio of 400 X.
- the invention surprisingly found that cyclohexenone compounds described herein effectively treat, inhibit and/or prevent fatty liver disease.
- treat means reducing the frequency, extent, severity and/or duration with which symptoms of fatty liver disease are experienced by a patient.
- the term “prevent,” “prevention” or “preventing” means inhibition, risk reduction, reducing the onset of or the averting of symptoms associated with fatty liver disease.
- pharmaceutically acceptable salt refers to those salts which retain the biological effectiveness and properties of the free bases and which are obtained by reaction with inorganic or organic acids such as hydrochloric acid, hydrobromic acid, sulfuric acid, nitric acid, phosphoric acid, methanesulfonic acid, ethanesulfonic acid, p-toluenesulfonic acid, salicylic acid, malic acid, maleic acid, succinic acid, tartaric acid, citric acid, and the like.
- the term "effective amount” means an amount of the compound described herein effective to treat, inhibit and/or prevent fatty liver diseases.
- the effective amount of the compound described herein reduces the number of fat cells; reduces the liver size; inhibits (i.e., slow to some extent and preferably stop) fatty cell infiltration; inhibits (i.e., slows at least to some extent and preferably stops) inflammation (hepatitis), scarring (cirrhosis) or necrosis; and/or relieves to some extent one or more of the symptoms associated with the disease.
- Antrodia camphorata is also called Chang-Zhi, Niu Chang-Gu, red camphor mushroom and the like, which is a perennial mushroom belonging to the order Aphyllophorales, the family Polyporaceae. It is an endemic species in Taiwan growing on the inner rotten heart wood wall of Cinnamomum kanehirae Hay. C. kanehirai Hay is rarely distributed and being overcut unlawfully, which makes A. camphorata growing inside the tree in the wild became even rare. The price of A. camphorata is very expensive due to the extremely slow growth rate of natural A. camphorata that only grows between Junes to October. Traditionally, A. camphorata is used as a Chinese remedy for food, alcohol, and drug
- Triterpenoids are the most studied component among the numerous compositions of A. camphorata.
- US 7,385,088 is directed to a novel compound and use thereof, in particular to
- US 7,342,137 provides cyclohexenone compounds and their uses in tumor growth inhibition, which is an extract isolated and purified from A.
- camphorate in particular to 4-hydroxy-2,3-dimethoxy-6-methyl-5(3,7,l 1-trimethyl-dodeca- 2,6,10-trienyl)-cyclohex-2-enone. Furthermore, several uses of the compound, 4-hydroxy-2,3- dimethoxy-6-methyl-5(3 ,7, 11 -trimethyl-dodeca-2,6, 10-trienyl)-cyclohex-2-enone were developed. US 7,411,003 discloses the use of 4-hydroxy-2,3-dimethoxy-6-methyl-5(3,7,l 1- trimethyl-dodeca-2,6,10-trienyl)-cyclohex-2-enone in inhibiting HBV.
- US 7,456,225 discloses the use of 4-hydroxy-2,3-dimethoxy-6-methyl-5(3,7,l 1 -trimethyl-dodeca-2,6, 10-trienyl)- cyclohex-2-enone in liver protection such as alleviating liver injury and fibrosis induced by chemicals and reduces the serum levels of alanine aminotransferase (ALT) and aspartate aminotransferase (AST).
- ALT alanine aminotransferase
- AST aspartate aminotransferase
- US 7,468,392 discloses the use of 4-hydroxy-2,3-dimethoxy-6-methyl- 5(3,7,1 l-trimethyl-dodeca-2,6-10-trienyl)-cyclohex-2-enone in delaying fatigue.
- US 7,501,454 relates to the use of 4-hydroxy-2,3-dimethoxy-6-methyl-5(3,7,l l-trimethyl-dodeca-2,6,10- trienyl- )-cyclohex-2-enone in treating autoimmune diseases.
- US 8,236,860 provides the use of 4-hydroxy-2,3-dimethoxy-6-methyl-5-(3,7,l l-trimethyl-dodeca-2,6,10-trienyl)-cyclohex-2- enone in inhibiting the survival of pancreatic cancer cells.
- US 20110060055, US 20110060056, US 20110060057, US 20110060058 and US 20110060059 disclose the use of 4-hydroxy-2,3- dimethoxy-6-methyl-5(3,7,l l-trimethyl-dodeca-2,6,10-trienyl- )-cyclohex-2-enone in inhibiting the survival of lymphoma, gastric cancer, skin cancer, ovarian cancer and bladder cancer cells, respectively.
- the invention provides a method of treating, inhibiting and/or preventing fatty liver diseases in a patient in need thereof, comprising administering an effective amount of a cyclohexenone compound of the following formula (I) to said patient,
- each of X and Y independently is oxygen, NR 5 or sulfur;
- each of Ri, R 2 and R 3 independently is a hydrogen, methyl or (CH 2 ) m — CH 3 ;
- R 7 is a C r C 8 alkyl, OR 5 or NR5R5;
- n l-12; or a pharmaceutically acceptable salt, metabolite, solvate or prodrug thereof.
- the fatty liver diseases are the primary fatty liver diseases or the secondary fatty liver diseases.
- the secondary fatty liver disease is alcohol liver disease, fatty liver associated with chronic hepatitis infection, total parental nutrition (TPN), Reye's Syndrome, gastrointestinal disorders, or gastroparesis and irritable bowel (IBS) disorders.
- the fatty liver disease is cirrhosis or fibrosis.
- the cyclohexenone compound is prepared synthetically or semi-synthetically from any suitable starting material.
- the cyclohexenone compound is prepared by fermentation, or the like.
- Compound 1 also known as AntroquinonolTM or "Antroq”
- Compound 3 in some instances, is prepared from 4-hydroxy-2,3-dimethoxy-6-methylcyclohexa-2,5-dienone.
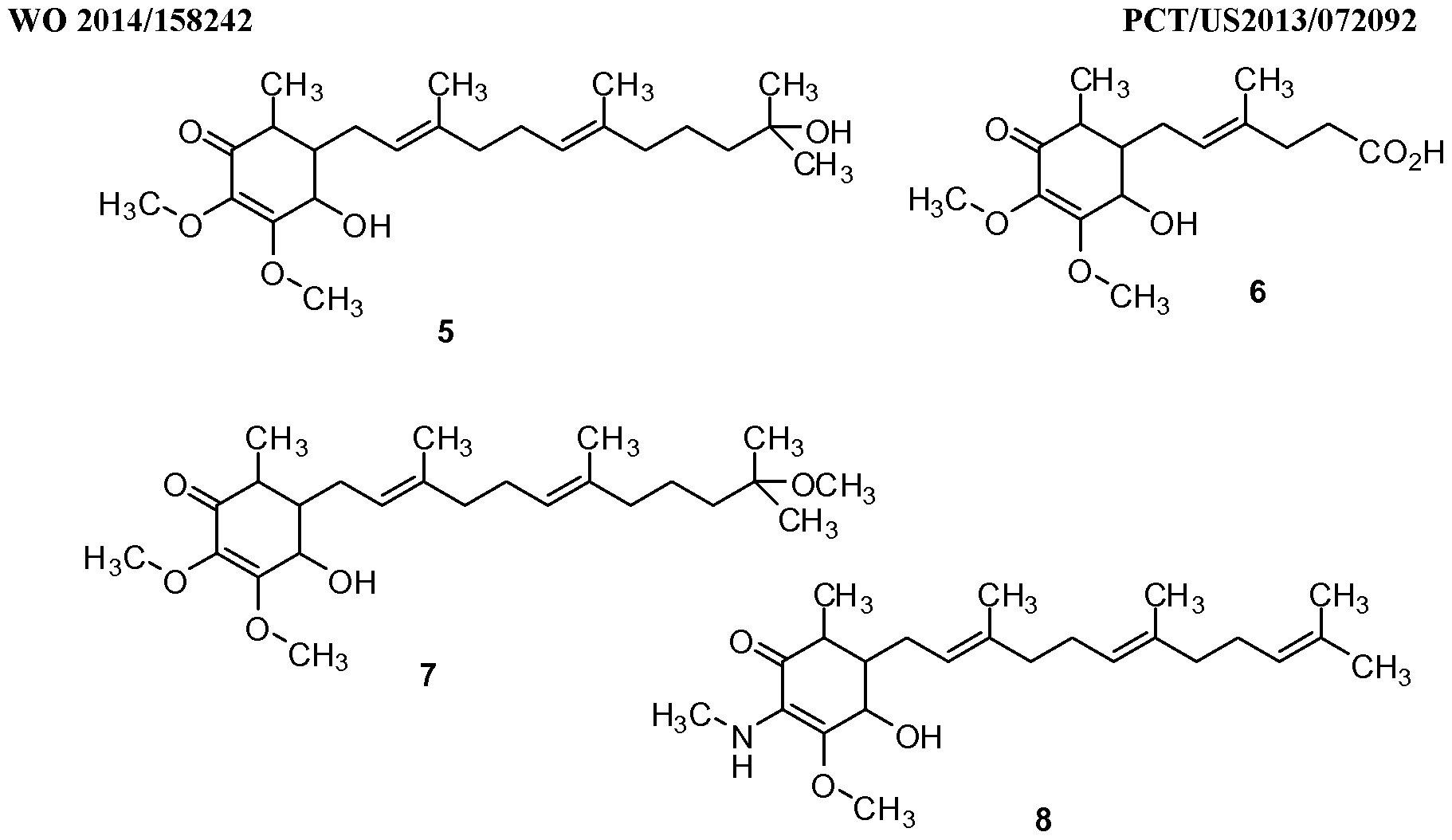
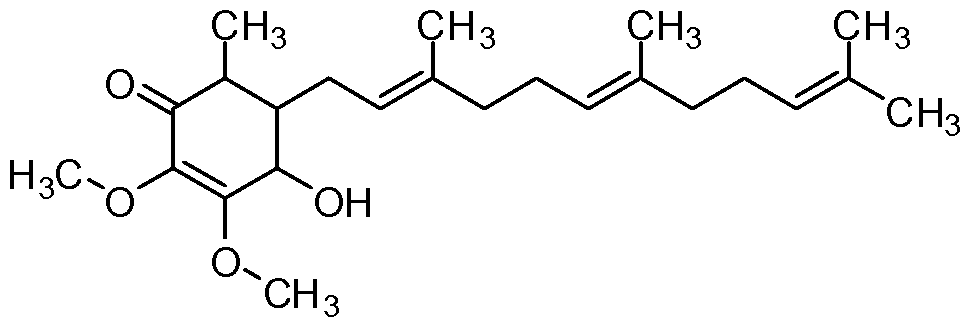
- the non-limited exemplary compounds are illustrated below.
- the organic solvent is selected from alcohols (e.g., methanol, ethanol, propanol, or the like), esters (e.g., methyl acetate, ethyl acetate, or the like), alkanes (e.g., pentane, hexane, heptane, or the like), halogenated alkanes (e.g., chloromethane, chloroethane, chloroform, methylene chloride, or the like), and the like.
- exemplary Compounds 1-7 are isolated from organic solvent extracts.
- the organic solvent is alcohol.
- the alcohol is ethanol.
- the organic solvent is selected from alcohols (e.g., methanol, ethanol, propanol, or the like), esters (e.g., methyl acetate, ethyl acetate, or the like), alkanes (e.g., pentane, hexane, heptane, or the like),
- cyclohexenone compound is isolated from the aqueous extracts of A. camphorata.
- Ri is a hydrogen or methyl.
- R 2 is a hydrogen, methyl, ethyl, propyl, butyl, pentyl or hexyl.
- R 3 is a hydrogen, methyl, ethyl, propyl, butyl, pentyl or hexyl.
- R 4 is
- the compound is
- the compounds provided herein are used in the treatment, inhibition and/or prevention of fatty liver disease.
- fatty liver diseases or liver disorders include the primary fatty liver diseases NAFLD and NASH and the secondary fatty liver diseases (e.g., alcoholic liver disease (ALD), fatty liver associated with chronic hepatitis infection, total parental nutrition (TPN), Reye's Syndrome, and gastrointestinal disorders such as Intestinal Bacterial Overgrowth (IBO), gastroparesis, irritable bowel (IBS) disorders, and the like).
- ALD alcoholic liver disease
- TPN total parental nutrition
- Reye's Syndrome e.g., Reye's Syndrome
- gastrointestinal disorders such as Intestinal Bacterial Overgrowth (IBO), gastroparesis, irritable bowel (IBS) disorders, and the like.
- therapeutically-effective dosages vary when the drugs are used in treatment combinations.
- Combination treatment further includes periodic treatments that start and stop at various times to assist with the clinical management of the patient.
- dosages of the co-administered compounds vary depending on the type of co-drug employed, on the specific drug employed, on the disease, disorder, or condition being treated and so forth.
- the dosage regimen to treat, prevent, or ameliorate the condition(s) for which relief is sought is modified in accordance with a variety of factors. These factors include the disorder from which the subject suffers, as well as the age, weight, sex, diet, and medical condition of the subject. Thus, in other embodiments, the dosage regimen actually employed varies widely and therefore deviates from the dosage regimens set forth herein.
- fatty liver disease therapeutic agents include, but are not limited to, the following: ergosterol, vitamin E, selenium, betaine, insulin sensitizers (e.g., Metformin, Pioglitazone, Rosiglitazone, Thiazolidinediones, or the like), and statins, or the like.
- the combinations of the cyclohexenone compounds and other fatty liver disease therapeutic agents described herein encompass additional therapies and treatment regimens with other agents in some embodiments.
- Such additional therapies and treatment regimens include another fatty liver disease therapy in some embodiments.
- additional therapies and treatment regimens include other agents used to treat adjunct conditions associated with fatty liver disease or a side effect from such agent in the combination therapy.
- adjuvants or enhancers are administered with a combination therapy described herein.
- the cyclohexenone compound of the invention is administered with a second ingredient.
- the second ingredient is ergosterol.
- the amounts of the cyclohexenone compound in combination with ergosterol range from 50% (w/w) to 90% (w/w) and 50%> (w/w) to 10%> (w/w), respectively.
- the compositions described herein and, in embodiments where combinational therapy is employed based on the mode of action described herein other agents do not have to be administered in the same pharmaceutical composition, and in some embodiments, because of different physical and chemical characteristics, are administered by different routes.
- the initial administration is made according to established protocols, and then, based upon the observed effects, the dosage, modes of administration and times of administration is modified by the skilled clinician.
- the compounds provided herein are administered by any convenient route, including oral, parenteral, subcutaneous, intravenous, intramuscular, intra peritoneal, or transdermal.
- the dosage administered depends upon the age, health, and weight of the recipient, kind of concurrent treatment, if any, and the nature of the effect desired.
- the compounds provided herein are mixed with one or more physiologically acceptable carriers comprising excipients and auxiliaries, which facilitate processing of the active compounds into preparations which are used
- the compounds provided herein are formulated as discrete units such as capsules, cachets or tablets each containing a predetermined amount of the compound of the invention; as a powder or granules; as solution or a suspension in an aqueous liquid or a non-aqueous liquid; or as an oil-in-water liquid emulsion or a water-in- oil liquid emulsion.
- the compounds provided herein are formulated in aqueous solutions, preferably in physiologically compatible buffers such as Hank's solution, Ringer's solution, or physiological saline buffer.
- physiologically compatible buffers such as Hank's solution, Ringer's solution, or physiological saline buffer.
- penetrants appropriate to the barrier to be permeated are used in the formulation.
- penetrants for example polyethylene glycol, are generally known in the art.
- pharmaceutical compositions which are used orally include push-fit capsules.
- the molecules for use according to the present invention are conveniently delivered in the form of an aerosol spray presentation from a pressurized pack or a nebulizer with the use of a suitable propellant, e.g.,
- the dosage unit is determined by providing a valve to deliver a metered amount in some embodiments.
- Capsules and cartridges of, e.g., gelatin for use in an inhaler or insufflator, is formulated containing a powder mix of the polypeptide and a suitable powder base such as lactose or starch in some embodiments.
- the dose will be determined by the activity of the compound produced and the condition of the subject, as well as the body weight or surface area of the subject to be treated.
- the size of the dose and the dosing regiment also will be determined by the existence, nature, and extent of any adverse side effects that accompany the administration of a particular compound in a particular subject.
- the physician In determining the effective amount of the compound to be administered, the physician needs to evaluate circulating plasma levels, toxicity, and progression of the disease.
- Example 1 Isolation of exemplary cvclohexenone compounds
- the HPLC was performed using a RP18 column, methanol (A) and 0.1-0.5% acetic acid (B) as the mobile phase, with gradient of 0-10 min in 95% ⁇ 20% B, 10-20 min in 20% ⁇ 10% B, 20-35 min in 10% - 10% B, 35-40 min in 10% - 95% B, at a flow rate of 1 ml/min.
- the effluent was monitored with a UV-visible detector.
- Compound 6 a metabolite of Compound 1, was obtained from urine samples of rats fed with Compound 1 in the animal study.
- Compound 6 was determined to be 4-hydroxy-2,3- dimethoxy-6-methyl-5-(3-methyl-2-hexenoic acid)cyclohex-2-enone with molecular weight of 312 (Ci6 H 24 0 6 ).
- the exemplary compounds may be prepared from 4-hydroxy-2,3- dimethoxy-6-methylcyclohexa-2,5-dienone, or the like.
- other cyclohexenone compounds having the structure
- Example 2 Reduction of Fatty Liver Condition by Compound 1 (4-hvdroxy-2,3-dimethoxy- 6-methyl-5 (3,7,11 -trimethyl-dodeca-2,6- 10-trienvD-cvclohex-2-enone)
- the example constructs an animal model using rats fed a high fat diet to evaluate the effects of chronic liver injury. Thereafter, the effects can be revealed through biochemical assays to prove the fatty liver reduction of exemplary compounds provided herein such as Compound 1, 4-hydroxy-2,3-dimethoxy-6-methyl-5(3,7,l 1 -trimethyl-dodeca-2,6- 10- trienyl)-cyclohex-2-enone (the test compound).
- the assay simulates liver disease caused by a high fat diet through a "Metabolic Syndrome" model. That is, the model is different from conventional chemical induced models caused by toxic components such as CC1 4 . This model is distinguishable from the models caused by virus or alcohol.
- mice were obtained from Charles River Laboratories Japan (Kanagawa, Japan). Animals were housed under specific-pathogen-free (SPF) conditions. The liver injury was developed in 18 male mice by subcutaneous injection of Streptozotocin (STZ) 2 days after birth (day 2). After 4 weeks, a high-fat commercial rodent diet ad libitum (CLEA JAPAN) were supplied. These mice were randomized into 3 groups before the treatment. The test compound was administered in a volume of 10 ml/kg twice a day for three weeks. In the control group (group A), six rats were fed with vehicle (corn oil from Sigma Chemical Co.) via intubation. Six mice in group B were orally administered vehicle and the test compound at a dose of 48 mg/kg twice a day (96 mg/kg per day). Table 1 summarizes the study timetable. Table 1
- Table 2 summarizes the treatment schedule.
- HE Staining The HE staining method is performed as follows: Liver slices are cut from the livers' left side, embedded in Tissue-Tek® OCTTM Compounds (Sakura Finetek, Japan), snap frozen in liquid nitrogen, and stored at -80°C. 5 ⁇ sections are cut, air-dried, fixed in acetone, air dried again and finally washed with phosphate buffered saline (PBS).
- PBS phosphate buffered saline
- liver sections will be prefixed in a Bouin solution (formalin-acetic acid) for one week and then stained with Lillie-Mayer's Hematoxylin (Muto Pure Chemicals, Japan) and eosin solution (Wako, Japan) to visualize the lipid deposition, inflammations, cell necrosis and fibrosis, or stained with Masson's trichromic solution to visualize extra cellular matrix and collagen fibers of liver fibrosis development.
- Bouin solution formalin-acetic acid
- the Sirius Red staining method is performed as follows: Liver slices are cut from the livers' left side, embedded in Tissue-Tek® OCTTM Compounds (Sakura Finetek, Japan), snap frozen in liquid nitrogen, and stored at -80°C. 5 ⁇ sections are cut, air- dried, fixed in acetone, air dried again and finally washed with phosphate buffered saline (PBS). Then, liver sections are stained with a Picro-Sirius Red Solution (Waldeck GmbH & KG, Germany) to observe collagen deposition.
- PBS phosphate buffered saline
- AST Plasma Aspartate aminotransferase
- ALT Alanine aminotransferase
- Blood samples were collected in heparinized syringes (Novo-Heparin 5,000 units/5 ml, Mochida Pharmaceutical, Japan) by cardiac puncture and kept on ice then centrifuged at 1,000 x g at 4°C for 15 minutes. The supernatant was collected and stored at -80°C until use.
- AST, ALT levels were measured by FUJI DRY CHEM 7000 (Fuji Film, Japan).
- FIG. 1 to FIG. 7 have proved that the exemplary compound extracted from A.
- camphorata (Compound 1) effectively decreases the extent of fatty liver disease caused by non- chemical injury.
- the decrease is assessed by evaluating the extent of liver injuries of fat deposition by histological analyses such as HE staining, Sirius red staining and collagen immunostaining, and further by plasma biochemical marker such as blood glucose, plasma triglyceride, plasma ALT and plasma AST.
- FIG. 1(A-D) shows the representative photomicrographs of HE-stained sections of livers of Group A and Group B, wherein FIG. 1(A) and 1(C) show an enlargement ratio of 50 X and FIG. 1(B) and 1(D) show an enlargement ratio of 200 X.
- the Group A (vehicle) diagrams revealed infiltration of inflammatory cells, macro- and micro vesicular fat deposition, proliferated bile ducts and hepato-cellular ballooning in the liver sections.
- group B the test compound, Compound 1 treatment tended to decrease the infiltration of inflammatory cells and also tended to decrease the macro-vesicular fat deposition compared to Group A.
- FIG. 2 shows the representative photomicrographs of Sirius-red staining of livers of Group A and Group B, wherein FIG. 2(A) and 2(C) show an enlargement ratio of 50 X and FIG. 2(B) and 2(D) show an enlargement ratio of 200 X.
- FIG. 2(A) and 2(B) in group A, Sirius red staining demonstrates collagen deposition around central veins, bile ducts and degenerative hepatocytes.
- FIG. 2(C) and 2(D) treatment the collagen deposition around the central veins and the bile ducts was reduced.
- FIG. 3 shows the representative photomicrographs of collagen Type 3-immunostained sections of livers of Group A and Group B, wherein FIG. 3(A) and 3(C) show an enlargement ratio of 50 X and FIG. 3(B) and 3(D) show an enlargement ratio of 400 X.
- Collagen Type 3 staining shows accumulation of collagen fibers in the sinusoidal area and around bile ducts and central veins in the Vehicle control group A.
- the Group B the test compound, Compound 1 treatment tended to reduce the thickness and/or the length of the collagen fibers in the sinusoidal area.
- FIG. 4 shows the diagram of the whole blood glucose concentration (mg/dL) of Group A and Group B.
- Group B treatment the test compound, Compound 1
- Group A 636 ⁇ 137 mg/dL
- Group B 580 ⁇ 122 mg/dL
- FIG. 5 shows the diagram of the plasma triglyceride (TG) concentration (mg/dL) of Group A and Group B.
- TG plasma triglyceride
- AST and ALT are important enzymes in the amino acid synthesis for the human organs such as liver, heart, muscles, etc.
- AST and ALT are commonly measured clinically as a part of a diagnostic evaluation of hepatocellular injury, to determine liver health. These enzymes' content in serum is low under normal conditions. Significantly elevated levels of AST and ALT often suggest the existence of liver injury.
- FIG. 6 and FIG. 7 show diagrams of plasma AST and plasma ALT concentration (U/dL) for Group A and Group B, respectively. As shown in FIG.
- Group B (the test compound, Compound 1) treatment seems to slightly reduce the plasma AST level compared to Group A (vehicle) treatment (Group A: 202 ⁇ 177 U/L, Group B: 141 ⁇ 35 U/L).
- Group B (the test compound, Compound 1) treatment seems to slightly reduce the plasma ALT level compared to Group A (vehicle) treatment (Group A: 64 ⁇ 64 U/L, Group B: 34 ⁇ 10 U/L).
- test compound treatment decreased the plasma TG levels, tending to inhibit blood glucose levels, and slightly decreased the plasma AST and ALT.
- the test compound treatment also decreased the infiltration of inflammatory cells and fat deposition in the liver lobule.
- the test compound tended to inhibit collagen deposition, shown in both Sirius red staining and collagen Type 3 staining, suggesting that the test compound has an anti-fibrotic effect on liver fibrosis steatohepatitis.
- FIG. 8 to FIG. 14 show that the test compound, Compound 1 effectively decrease fibrosis of steatohepatitis liver cells induced by non-chemical injury.
- the decrease is assessed by evaluating the extent of liver injuries in liver fibrosis by histological analyses such as HE staining, Sirius red staining and collagen immunostaining, and further by plasma biochemical marker such as blood glucose, plasma alanine aminotransferase and plasma aspartate
- FIG. 8 shows the representative photomicrographs of HE-stained sections of livers of Group A and Group B, wherein FIG. 8(A) and 8(C) show an enlargement ratio of 50 X, and FIG. 8(B) and 8(D) show an enlargement ratio of 200 X.
- the Group A (vehicle) diagrams reveal infiltration of inflammatory cells, macro- and micro vesicular fat deposition, proliferated bile ducts, and hepatocellular ballooning in the liver sections.
- group B the test compound, Compound 1 treatment tended to decrease the macro -vesicular fat deposition compared to Group A.
- FIG. 9 shows the representative photomicrographs of Sirius-red staining of livers of Group A and Group B, wherein FIG. 9(A) and 9(C) show an enlargement ratio of 50 X, and FIG. 9(B) and 9(D) show an enlargement ratio of 200 X.
- FIG. 9(A) and 9(B) in Group A, Sirius red staining demonstrates collagen deposition around central veins, bile ducts and degenerative hepatocytes.
- Group A treatment central-to-central bridging fibrosis is observed, showing serious fibrosis in liver cells.
- FIG. 9(C) and 9(D) treatment the collagen deposition around the central veins and the bile ducts was reduced.
- FIG. 10 shows the representative photomicrographs of collagen Type 3-immunostained sections of livers of Group A and Group B, wherein FIG. 10(A) and 10(C) show an enlargement ratio of 50 X, and FIG. 10(B) and 10(D) show an enlargement ratio of 400 X.
- Collagen Type 3 staining shows accumulation of collagen fibers in the sinusoidal area, and around bile ducts and central veins in the Vehicle control Group A.
- the Group B the test compound, Compound 1 treatment tended to reduce the thickness and/or the length of the collagen fibers in the sinusoidal area.
- FIG. 11 shows the diagram of the whole blood glucose concentration (mg/dL) of Group A and Group B.
- Group B treatment the test compound, Compound 1
- Group A 728 ⁇ 109 mg/dL
- Group B 566 ⁇ 65 mg/dL
- FIG. 12 shows the diagram of the plasma triglyceride (TG) concentration (mg/dL) of Group A and Group B. As shown in FIG. 12, Group B treatment (the test compound,
- Compound 1 showed a slight decrease in the plasma TG compared to the results of Group A treatment (Group A: 758 ⁇ 877 mg/dL, Group B : 704 ⁇ 450 mg/dL).
- FIG. 13 and FIG. 14, respectively show diagrams of plasma AST and plasma ALT concentration (U/dL) for Group A and Group B.
- Group B the test compound, Compound 1 treatment slightly increase the plasma AST level compared to Group A (vehicle) treatment, but the change is not significant (Group A: 143 ⁇ 42 U/L, Group B: 167 ⁇ 87 U/L).
- Group B the test compound, Compound 1 treatment reduces the plasma ALT level compared to Group A (vehicle) treatment (Group A: 47 ⁇ 22 U/L, Group B: 38 ⁇ 11 U/L).
- the treatment with the test compound decreased the blood glucose levels, the plasma TG levels, and tends to decrease the fat deposition in the liver lobule and the ALT levels, suggesting that the cyclohexenone compounds provided herein have an ameliorating effect on lipid and carbohydrate metabolism and a protective effect on liver injury caused by a high-fat diet.
- the exemplary cyclohexenone compound e.g.,
- Compound 1 tended to inhibit collagen deposition, shown in both Sirus red staining and collagen Type 3 staining, showing that the cyclohexenone compounds provided herein have an anti-fibrotic effect on liver steatohepatitis.
- Example 3 Reduction of Fatty Liver Condition by the composition comprising Compound 1 and ergosterol
- control group (group A), six rats were fed with vehicle (corn oil from Sigma chemical co.) by means of stomach tubes.
- Six rats in group B were orally administered vehicle and the test compound (Compound 1) at a dose of 48 mg/kg twice a day (96 mg/kg per day) and ergosterol at a dose of 12 mg/kg twice a day (24 mg/kg per day).
- Six mice in group C were orally administered vehicle and the test compound (Compound 1) at a dose of 48 mg/kg twice a day (96 mg/kg per day).
- Table 1 below shows the study timetable summary.
- Table 2 shows the treatment schedule.
- FIG. 15 shows the representative photomicrographs of HE-stained sections of livers from Group A to Group C, wherein FIG. 15(A), 15(C), 15(E) show an enlargement ratio of 50 X and FIG. 15(B), 15(D), 15(F) show an enlargement ratio of 200 X.
- FIG. 15(A) and 15(B) the Group A figures revealed infiltration of inflammatory cells, macro- and micro vesicular fat deposition, proliferated bile ducts and hepatocellular ballooning in the liver sections.
- FIG. 15(A), 15(C), 15(E) show an enlargement ratio of 50 X
- FIG. 15(B) shows an enlargement ratio of 200 X.
- the Group A figures revealed infiltration of inflammatory cells, macro- and micro vesicular fat deposition, proliferated bile ducts and hepatocellular ballooning in the liver sections.
- FIG. 15(A) and 15(B) the Group A figures revealed infiltration of
- treatment with combination of the test compound (Compound 1) and ergosterol decreased the macro vesicular fat deposition and the infiltration of inflammatory cells.
- the number of mitotic figures in hepatocytes is higher in group B compared to the group A.
- the treatment with the test compound alone tended to decrease the macro vesicular fat deposition but did not affect the infiltration of inflammatory cells.
- the treatment with the test compound and ergosterol (Group B) further inhibit the inflammatory cells infiltration, thereby showing better anti-inflammatory effects with respect to Group C.
- FIG. 16 shows the representative photomicrographs of Sirius-red stained of livers from Group A to Group C, wherein FIG. 16(A), 16(C), 16(E) show an enlargement ratio of 50 X and FIG. 16(B), 16(D), 16(F) show an enlargement ratio of 200 X.
- FIG. 16(A) and 16(B) in group A, Sirius red staining show collagen deposition around central veins, bile ducts and degenerative hepatocytes, showing central-to-central bridging fibrosis and indicating serious fibrosis steatohepatitis.
- FIG. 16 shows the representative photomicrographs of Sirius-red stained of livers from Group A to Group C, wherein FIG. 16(A), 16(C), 16(E) show an enlargement ratio of 50 X and FIG. 16(B), 16(D), 16(F) show an enlargement ratio of 200 X.
- Sirius red staining show collagen deposition around central veins, bil
- both the treatments with the cyclohexeone compound provided herein (e.g., Compound 1) and ergosterol treatment (Group B) and the treatment with the test compound alone (Group C) tend to inhibit collagen deposition, and thus prevent liver fibrosis. More specifically, the treatment with the combination of the cyclohexenone compound provided herein (e.g., Compound 1) and ergosterol provides a better anti-liver-fibrosis ability compared to the treatment with the test compound alone.
- FIG. 17 shows the representative photomicrographs of collagen Type 3-immunostained sections of livers from Group A to Group C, wherein FIG. 17(A), 17(C), 17(E) show an enlargement ratio of 100 X and FIG. 17(B), 17(D), 17(F) show an enlargement ratio of 400 X.
- Collagen Type 3 staining shows accumulation of collagen fibers in the sinusoidal area and around bile ducts and central veins in the Vehicle control group.
- FIG. 17(A), 17(C), 17(E) show an enlargement ratio of 100 X
- FIG. 17(B) show an enlargement ratio of 400 X.
- Collagen Type 3 staining shows accumulation of collagen fibers in the sinusoidal area and around bile ducts and central veins in the Vehicle control group.
- Example 4 Study of Compound 1 in Patients With Diabetes and Presumed NAFLD
- the primary objectives of this study are to assess, in patients with Type 2 diabetes mellitus (DM) and presumed nonalcoholic fatty liver disease (NAFLD), the following:
- homeostasis will be attained by performing a euglycemic clamp procedure at baseline (Day 0) and at the end of 6 weeks of treatment (Day 43).
- Hepatocellular Function [ Time Frame: baseline and 6 weeks ] [ Designated as safety issue: Yes ] [0095] Hepatocellular function as measured by assessment of liver enzymes and biochemical markers of hepatic and metabolic function
- Type 2 diabetes defined by the American Diabetes Association (ADA), as one of the following criteria:
- GTT oral glucose tolerance test
- Presumed NAFLD defined by one of the following criteria:
- a pharmaceutical composition for oral delivery 100 mg of an exemplary Compound 1 is mixed with 100 mg of corn oil. The mixture is incorporated into an oral dosage unit in a capsule, which is suitable for oral administration.
- 100 mg of a compound described herein is mixed with 750 mg of starch.
- the mixture is incorporated into an oral dosage unit for, such as a hard gelatin capsule, which is suitable for oral administration.
- a pharmaceutical composition for buccal delivery such as a hard lozenge
- a pharmaceutical composition for buccal delivery such as a hard lozenge
- the mixture is gently blended and poured into a mold to form a lozenge suitable for buccal administration.
- a pharmaceutical composition for inhalation delivery 20 mg of a compound described herein is mixed with 50 mg of anhydrous citric acid and 100 mL of 0.9% sodium chloride solution. The mixture is incorporated into an inhalation delivery unit, such as a nebulizer, which is suitable for inhalation administration.
- an inhalation delivery unit such as a nebulizer
Landscapes
- Health & Medical Sciences (AREA)
- Life Sciences & Earth Sciences (AREA)
- Chemical & Material Sciences (AREA)
- Veterinary Medicine (AREA)
- General Health & Medical Sciences (AREA)
- Animal Behavior & Ethology (AREA)
- Public Health (AREA)
- Medicinal Chemistry (AREA)
- Pharmacology & Pharmacy (AREA)
- Epidemiology (AREA)
- Engineering & Computer Science (AREA)
- Bioinformatics & Cheminformatics (AREA)
- Natural Medicines & Medicinal Plants (AREA)
- Zoology (AREA)
- Botany (AREA)
- Mycology (AREA)
- Organic Chemistry (AREA)
- Chemical Kinetics & Catalysis (AREA)
- Nuclear Medicine, Radiotherapy & Molecular Imaging (AREA)
- General Chemical & Material Sciences (AREA)
- Alternative & Traditional Medicine (AREA)
- Biotechnology (AREA)
- Otolaryngology (AREA)
- Pulmonology (AREA)
- Nutrition Science (AREA)
- Microbiology (AREA)
- Physiology (AREA)
- Dispersion Chemistry (AREA)
- Medical Informatics (AREA)
- Gastroenterology & Hepatology (AREA)
- Acyclic And Carbocyclic Compounds In Medicinal Compositions (AREA)
- Pharmaceuticals Containing Other Organic And Inorganic Compounds (AREA)
- Medicines That Contain Protein Lipid Enzymes And Other Medicines (AREA)
- Medicines Containing Plant Substances (AREA)
- Organic Low-Molecular-Weight Compounds And Preparation Thereof (AREA)
Abstract
Description
Claims
Priority Applications (9)
| Application Number | Priority Date | Filing Date | Title |
|---|---|---|---|
| SG11201507181YA SG11201507181YA (en) | 2013-03-13 | 2013-11-26 | Method for the treatment of fatty liver disease |
| BR112015022571A BR112015022571A2 (en) | 2013-03-13 | 2013-11-26 | Liver steatosis treatment method |
| CN201380074591.0A CN105209028B (en) | 2013-03-13 | 2013-11-26 | Methods of treating fatty liver disease |
| KR1020157027353A KR20150130352A (en) | 2013-03-13 | 2013-11-26 | Method for the treatment of fatty liver disease |
| MX2015012455A MX2015012455A (en) | 2013-03-13 | 2013-11-26 | Method for the treatment of fatty liver disease. |
| HK16104631.9A HK1216614B (en) | 2013-03-13 | 2013-11-26 | Method for the treatment of fatty liver disease |
| ES13880440T ES2730739T3 (en) | 2013-03-13 | 2013-11-26 | Cyclohexenone compounds for the treatment of fatty liver disease |
| EP13880440.6A EP2968217B1 (en) | 2013-03-13 | 2013-11-26 | Cyclohexenone compounds for treating fatty liver disease |
| JP2016500112A JP6377713B2 (en) | 2013-03-13 | 2013-11-26 | Drug |
Applications Claiming Priority (2)
| Application Number | Priority Date | Filing Date | Title |
|---|---|---|---|
| US13/801,697 | 2013-03-13 | ||
| US13/801,697 US20140274979A1 (en) | 2013-03-13 | 2013-03-13 | Method for the treatment of fatty liver disease |
Publications (1)
| Publication Number | Publication Date |
|---|---|
| WO2014158242A1 true WO2014158242A1 (en) | 2014-10-02 |
Family
ID=51529924
Family Applications (1)
| Application Number | Title | Priority Date | Filing Date |
|---|---|---|---|
| PCT/US2013/072092 Ceased WO2014158242A1 (en) | 2013-03-13 | 2013-11-26 | Method for the treatment of fatty liver disease |
Country Status (11)
| Country | Link |
|---|---|
| US (4) | US20140274979A1 (en) |
| EP (1) | EP2968217B1 (en) |
| JP (1) | JP6377713B2 (en) |
| KR (1) | KR20150130352A (en) |
| CN (1) | CN105209028B (en) |
| BR (1) | BR112015022571A2 (en) |
| ES (1) | ES2730739T3 (en) |
| MX (1) | MX2015012455A (en) |
| SG (1) | SG11201507181YA (en) |
| TW (1) | TWI631943B (en) |
| WO (1) | WO2014158242A1 (en) |
Cited By (2)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| JP2018534323A (en) * | 2015-11-19 | 2018-11-22 | シニュー・ファーマ・インコーポレイテッドSiNew Pharma Inc. | Pharmaceutical composition for prevention or treatment of fatty liver |
| JP2019529563A (en) * | 2016-09-23 | 2019-10-17 | パーデュー・リサーチ・ファウンデーションPurdue Research Foundation | Anticancer agent and preparation method thereof |
Families Citing this family (3)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| CN107343890A (en) * | 2016-05-06 | 2017-11-14 | 北京大学 | The application of Antrodia camphorata and monomer lanostane 32 in NASH is prevented and treated |
| MY194948A (en) * | 2016-05-13 | 2022-12-28 | Golden Biotechnology Corp | Methods and compositions for treating advanced stage non-small cell lung cancer |
| US11253527B2 (en) * | 2019-02-25 | 2022-02-22 | Arjil Biotech Holding Company Limited | Method and composition for inhibiting virus infection |
Citations (3)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| US20080312335A1 (en) * | 2007-06-14 | 2008-12-18 | Golden Biotechnology Corporation | Liver protection compounds of the cyclohexenone type from antrodia camphorata |
| US20090156614A1 (en) * | 2006-07-19 | 2009-06-18 | Dalton James T | Selective androgen receptor modulators, analogs and derivatives thereof and uses thereof |
| US20120071426A1 (en) * | 2010-09-20 | 2012-03-22 | Golden Biotechnology Corporation | Methods and compositions for treating lung cancer |
Family Cites Families (4)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| CN101516835A (en) * | 2006-07-19 | 2009-08-26 | 俄亥俄州立大学研究基金会 | Selective androgen receptor modulators, analogs and derivatives thereof and uses thereof |
| JP2008260695A (en) * | 2007-04-10 | 2008-10-30 | Nissei Bio Kk | Hepatopathy inhibitor |
| CN101785793A (en) * | 2009-01-23 | 2010-07-28 | 伟诚生物科技有限公司 | Uses of Antrodia Camphorata Extract Capsules for Protecting the Liver and Improving the Body's Immunological Regulatory Function |
| WO2011145340A1 (en) * | 2010-05-19 | 2011-11-24 | 興和株式会社 | Prophylactic and/or therapeutic agent for non-alcoholic steatohepatitis |
-
2013
- 2013-03-13 US US13/801,697 patent/US20140274979A1/en not_active Abandoned
- 2013-11-26 KR KR1020157027353A patent/KR20150130352A/en not_active Withdrawn
- 2013-11-26 MX MX2015012455A patent/MX2015012455A/en unknown
- 2013-11-26 WO PCT/US2013/072092 patent/WO2014158242A1/en not_active Ceased
- 2013-11-26 JP JP2016500112A patent/JP6377713B2/en active Active
- 2013-11-26 SG SG11201507181YA patent/SG11201507181YA/en unknown
- 2013-11-26 CN CN201380074591.0A patent/CN105209028B/en active Active
- 2013-11-26 BR BR112015022571A patent/BR112015022571A2/en not_active IP Right Cessation
- 2013-11-26 ES ES13880440T patent/ES2730739T3/en active Active
- 2013-11-26 EP EP13880440.6A patent/EP2968217B1/en active Active
-
2014
- 2014-01-09 TW TW103100845A patent/TWI631943B/en active
-
2017
- 2017-06-26 US US15/633,719 patent/US20170304224A1/en not_active Abandoned
-
2019
- 2019-11-29 US US16/699,405 patent/US10959963B2/en active Active
-
2021
- 2021-02-20 US US17/180,781 patent/US20210177775A1/en not_active Abandoned
Patent Citations (3)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| US20090156614A1 (en) * | 2006-07-19 | 2009-06-18 | Dalton James T | Selective androgen receptor modulators, analogs and derivatives thereof and uses thereof |
| US20080312335A1 (en) * | 2007-06-14 | 2008-12-18 | Golden Biotechnology Corporation | Liver protection compounds of the cyclohexenone type from antrodia camphorata |
| US20120071426A1 (en) * | 2010-09-20 | 2012-03-22 | Golden Biotechnology Corporation | Methods and compositions for treating lung cancer |
Non-Patent Citations (1)
| Title |
|---|
| AO, ZH ET AL.: "Niuchangchih (Antrodia camphorata) and its potential in treating liver diseases", JOUMAL OF ETHNOPHARMACOLOGY, vol. 121, 17 November 2008 (2008-11-17), pages 194 - 212, XP025842589 * |
Cited By (4)
| Publication number | Priority date | Publication date | Assignee | Title |
|---|---|---|---|---|
| JP2018534323A (en) * | 2015-11-19 | 2018-11-22 | シニュー・ファーマ・インコーポレイテッドSiNew Pharma Inc. | Pharmaceutical composition for prevention or treatment of fatty liver |
| JP2019529563A (en) * | 2016-09-23 | 2019-10-17 | パーデュー・リサーチ・ファウンデーションPurdue Research Foundation | Anticancer agent and preparation method thereof |
| JP7111722B2 (en) | 2016-09-23 | 2022-08-02 | パーデュー・リサーチ・ファウンデーション | ANTI-CANCER AGENT AND PREPARATION METHOD THEREOF |
| US11851441B2 (en) | 2016-09-23 | 2023-12-26 | Purdue Research Foundation | Anti-cancer agents and preparation thereof |
Also Published As
| Publication number | Publication date |
|---|---|
| US10959963B2 (en) | 2021-03-30 |
| TW201440759A (en) | 2014-11-01 |
| EP2968217B1 (en) | 2019-03-13 |
| US20170304224A1 (en) | 2017-10-26 |
| US20200093757A1 (en) | 2020-03-26 |
| JP2016512238A (en) | 2016-04-25 |
| US20140274979A1 (en) | 2014-09-18 |
| BR112015022571A2 (en) | 2017-07-18 |
| MX2015012455A (en) | 2016-04-07 |
| HK1216614A1 (en) | 2016-11-25 |
| EP2968217A4 (en) | 2016-11-02 |
| ES2730739T3 (en) | 2019-11-12 |
| SG11201507181YA (en) | 2015-10-29 |
| CN105209028B (en) | 2019-06-14 |
| CN105209028A (en) | 2015-12-30 |
| US20210177775A1 (en) | 2021-06-17 |
| KR20150130352A (en) | 2015-11-23 |
| EP2968217A1 (en) | 2016-01-20 |
| TWI631943B (en) | 2018-08-11 |
| JP6377713B2 (en) | 2018-08-22 |
Similar Documents
| Publication | Publication Date | Title |
|---|---|---|
| US10959963B2 (en) | Method for the treatment of fatty liver disease | |
| AU2021219903B2 (en) | Use of kaurane compounds in preparation of drug for prevention and treatment of sepsis and multiple organ damage | |
| KR101069959B1 (en) | Liver protection compounds of the cyclohexenone type from Antrodia camphorata | |
| AU2011230081A1 (en) | Pharmaceutical composition for the prevention or the treatment of non-alcoholic fatty liver disease and the method for prevention or treatment of non-alcoholic fatty liver disease using the same | |
| CN118178446A (en) | Application of triacetyl-3-hydroxyphenyladenosine in the preparation of drugs for preventing or treating non-alcoholic fatty liver disease | |
| US8927601B2 (en) | Uses of N-butylidenephthalide in treating a liver injury and improving liver function | |
| CN120417912A (en) | Pharmaceutical composition comprising sodium-glucose cotransporter 2 inhibitor and angiotensin II receptor blocker for preventing or treating nonalcoholic fatty liver disease | |
| SE1350211A1 (en) | Methods and compositions for the treatment of cancer metastases | |
| HK1216614B (en) | Method for the treatment of fatty liver disease | |
| CN114869870B (en) | Use of EPI-001 for preventing and/or treating nonalcoholic fatty liver disease | |
| KR101351406B1 (en) | A composition for athero-sclerosis comprising the polyphenol extracts from Phellinus baumii | |
| CN105273031B (en) | Novel triterpenes and uses thereof | |
| US20230190682A1 (en) | Pharmaceutical composition for preventing or treating metabolic diseases | |
| CN108283634A (en) | Chrysin and its derivative are preparing the purposes in preventing and treating fatty liver medicament | |
| JP2007031302A (en) | Adiponectin production accelerator and metabolic syndrome preventive | |
| KR20260033973A (en) | Composition for preventing or treating metabolic dysfunction-associated liver disease comprising Oenothein B | |
| KR20230008711A (en) | Methods and compositions for treating RNA virus induced diseases | |
| TW201503889A (en) | Use of eburicoic acid or derivative thereof in prevention or treatment of pain, inflammation and liver injury | |
| CN113082033A (en) | Application of FR180204 in preparation of medicine for preventing and/or treating non-alcoholic fatty liver disease or hepatitis | |
| CN109394740A (en) | Isoliquiritigenin, pharmaceutical composition and its application in preparation treatment diabetic cardiomyopathy drug | |
| US20150265644A1 (en) | Therapeutic methods and compositions for treating diabetes utilizing diterpenoid compounds | |
| US20090087497A1 (en) | Compositions and methods for treating symptoms of aging | |
| CA2847286A1 (en) | Therapeutic methods and compositions for treating diabetes utilizing diterpenoid compounds | |
| JP2000016946A (en) | Hyperglycemic inhibitor and hepatopathy inhibitor |
Legal Events
| Date | Code | Title | Description |
|---|---|---|---|
| 121 | Ep: the epo has been informed by wipo that ep was designated in this application |
Ref document number: 13880440 Country of ref document: EP Kind code of ref document: A1 |
|
| ENP | Entry into the national phase |
Ref document number: 2016500112 Country of ref document: JP Kind code of ref document: A |
|
| WWE | Wipo information: entry into national phase |
Ref document number: MX/A/2015/012455 Country of ref document: MX |
|
| NENP | Non-entry into the national phase |
Ref country code: DE |
|
| ENP | Entry into the national phase |
Ref document number: 20157027353 Country of ref document: KR Kind code of ref document: A |
|
| WWE | Wipo information: entry into national phase |
Ref document number: 2013880440 Country of ref document: EP |
|
| REG | Reference to national code |
Ref country code: BR Ref legal event code: B01A Ref document number: 112015022571 Country of ref document: BR |
|
| ENP | Entry into the national phase |
Ref document number: 112015022571 Country of ref document: BR Kind code of ref document: A2 Effective date: 20150911 |